Introduction
This is a great question! These two terms are often used interchangeably, but they’re not the same thing. The difference is subtle, important, and worth making explicit on your site.
Short answer (for orientation)
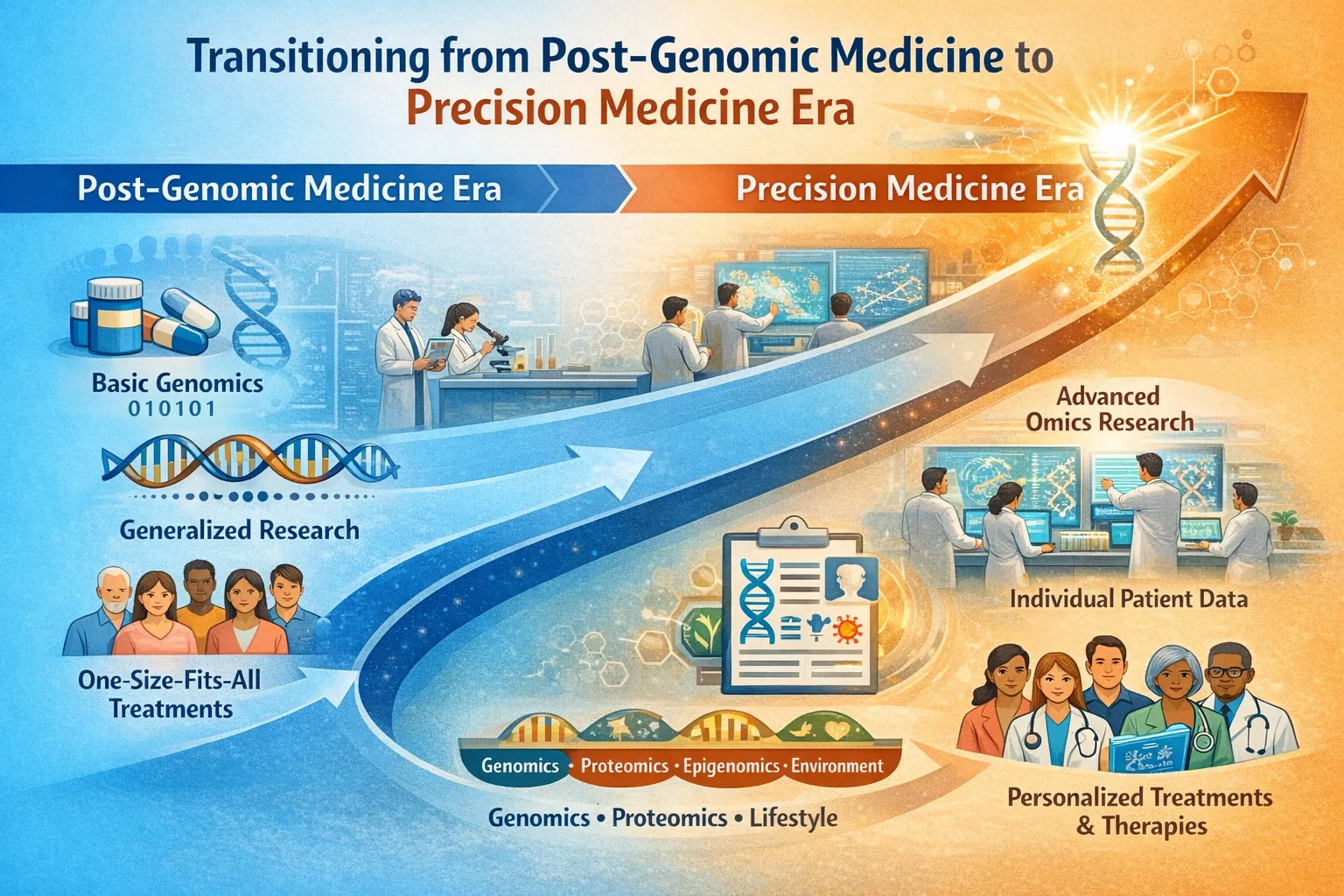
Post-genomic medicine describes our modern understanding of disease as a complex, context-dependent biological process. Precision medicine applies selected insights from this understanding to guide clinical decisions.
In other words:
Post-genomic medicine describes a historical and conceptual phase of medicine that comes after sequencing the human genome. Precision medicine is a clinical strategy that uses genomic (and other) data to tailor prevention and treatment to individuals or groupsPost-genomic medicine is the era. Precision medicine is one of its applications.
Post-genomic medicine
What it means
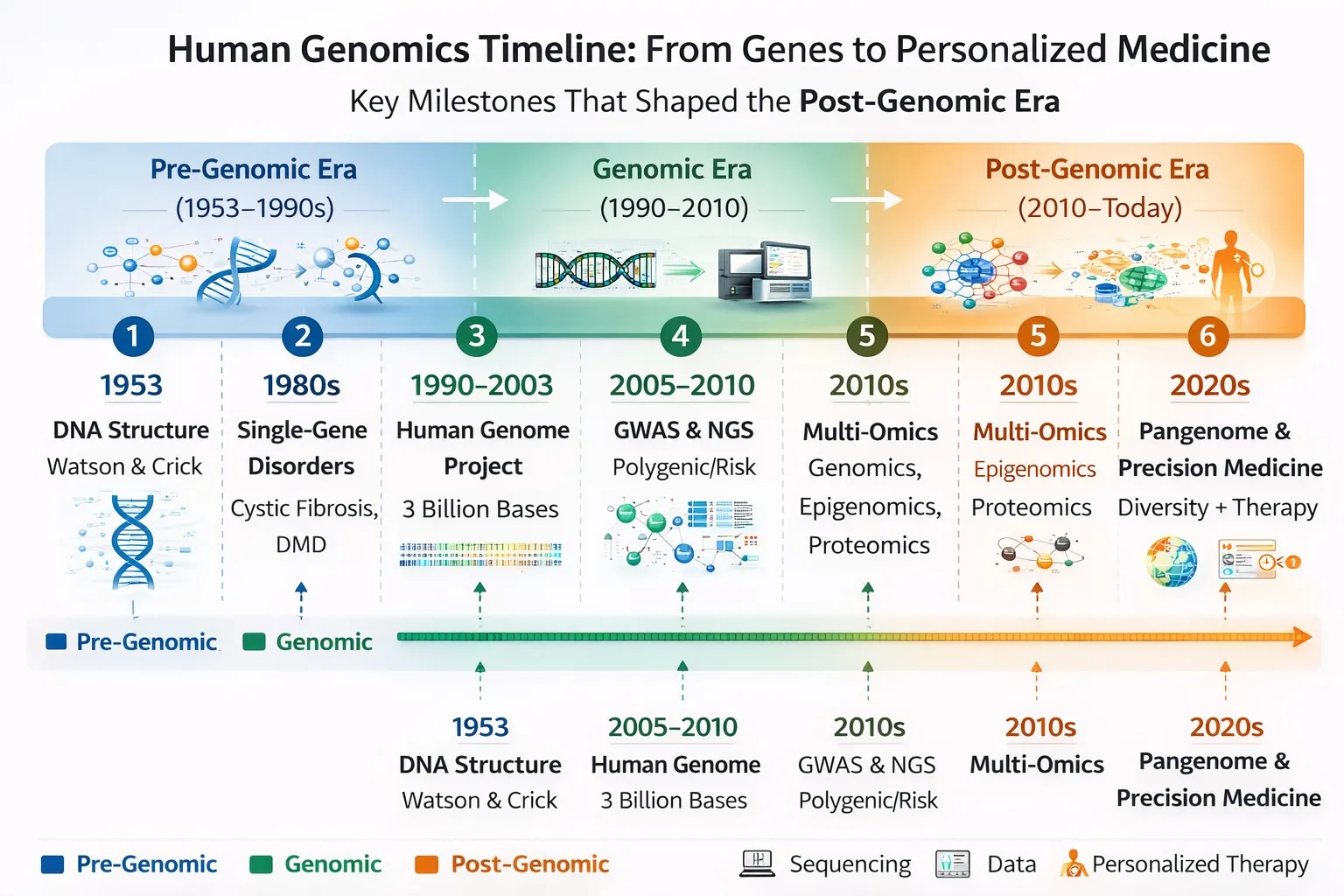
Post-genomic medicine refers to the period after the Human Genome Project, when it became clear that knowing the DNA sequence alone is not enough. Disease arises from complex interactions between:
- genes
- gene regulation
- environment
- immune responses
- development and time
It’s a way of thinking about biology and disease.
Core questions it asks
- Why do people with the same mutation have different outcomes?
- How do non-coding variants influence disease?
- How do immune context, epigenetics, and environment modify genetic risk?
Key characteristics
- Systems biology
- Multi-omics (genomics, transcriptomics, epigenomics, proteomics)
- Emphasis on context, regulation, and interaction
- Acceptance of uncertainty and probabilistic risk
What it is not
- Not a clinical program
- Not inherently personalised
- Not necessarily patient-facing
👉 Post-genomic medicine is the intellectual framework that replaced “one gene → one disease” thinking.
Precision medicine
What it means
Precision medicine is a clinical and translational approach that aims to:
Deliver the right intervention to the right patient at the right time based on biological, environmental, and lifestyle data.
Genomics is central—but not exclusive.
What data it uses
- Genomic variants
- Tumour mutations
- Immune profiles
- Biomarkers
- Imaging
- Lifestyle and environmental data
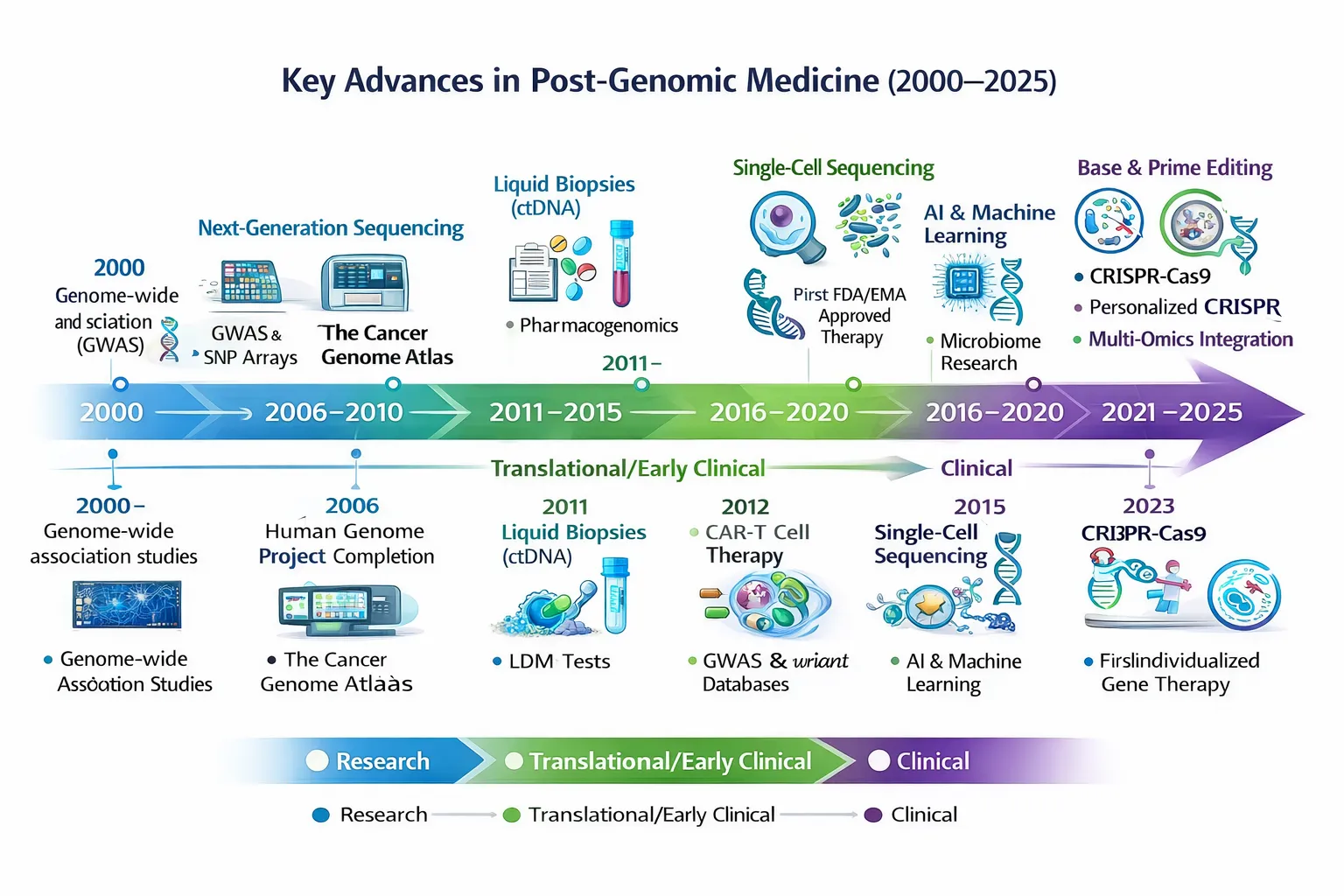
Typical examples
- Targeted cancer therapies
- Pharmacogenomics
- Polygenic risk stratification
- Biomarker-driven clinical trials
Defining feature
Actionability.
If it doesn’t change:
- diagnosis
- treatment
- prevention
- monitoring
…it’s not precision medicine, even if it’s genomics-heavy.
A prominent policy framing came from initiatives such as the Precision Medicine Initiative, which explicitly focused on translating biological insight into clinical care.
Side-by-side comparison
| Aspect | Post-Genomic Medicine | Precision Medicine |
|---|---|---|
| What it is | Scientific era & framework | Clinical strategy |
| Focus | Understanding biological complexity | Applying data to care |
| Core question | How does disease really work? | What should we do for this patient? |
| Timeframe | ~2003 onward | ~2010s onward |
| Output | Models, mechanisms, insights | Tests, therapies, stratification |
| Patient-facing? | Usually indirect | Yes |

How they relate (this is the key insight)
Precision medicine depends on post-genomic medicine.
- Post-genomic research reveals complexity
- Precision medicine decides which complexity is clinically useful
Many failures of precision medicine happen when:
- We skip post-genomic understanding
- We overinterpret weak signals
- We mistake association for causation
Post-genomic medicine explains why medicine is hard. Precision medicine tries to make it useful anyway.