Introduction
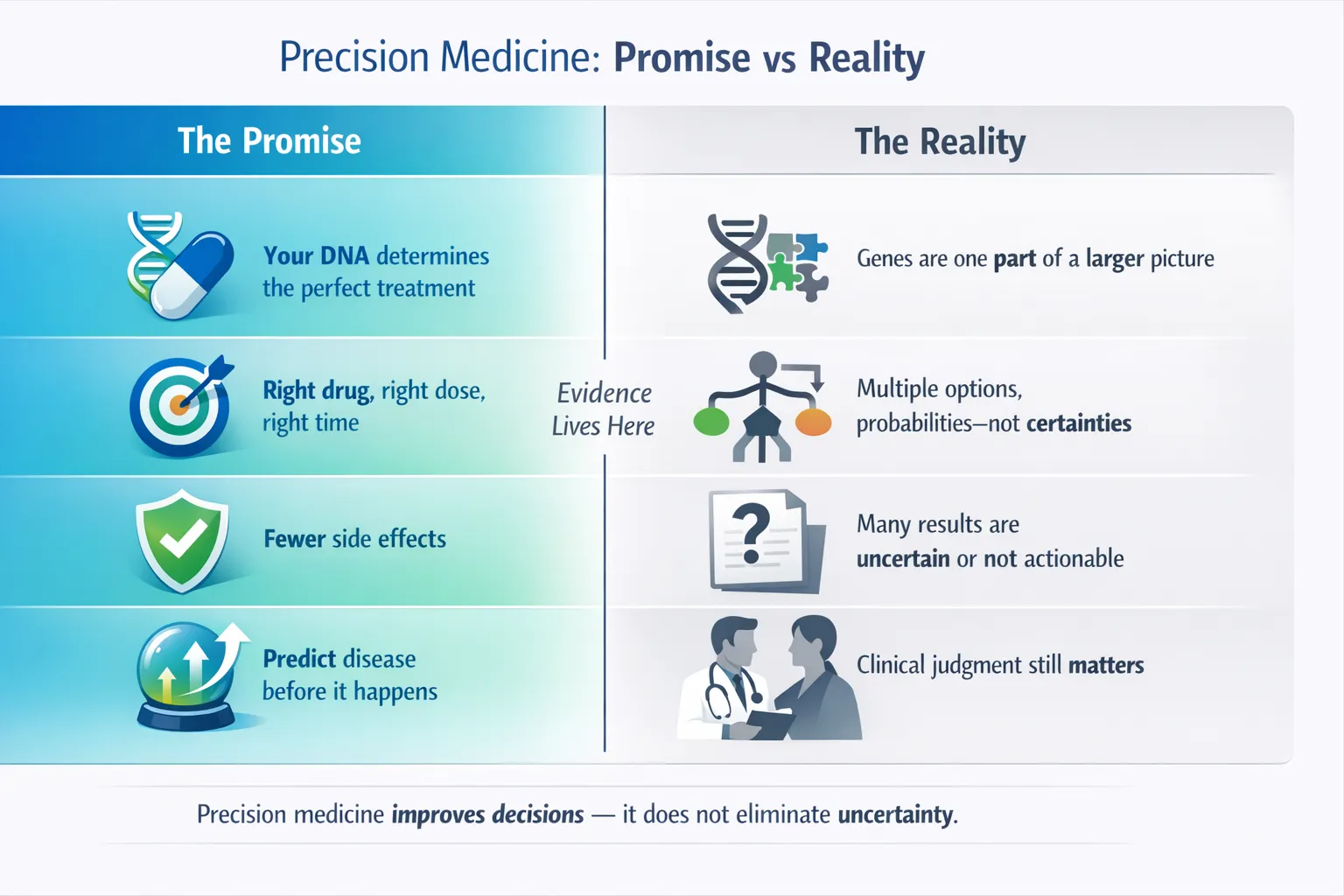
Precision medicine is transforming healthcare—but it is often misunderstood. Headlines promise perfectly tailored treatments and DNA-guided cures, while reality is more nuanced, more powerful, and more limited than hype suggests.
This article explains what precision medicine already does well, where it still falls short, and why both matter for patients and clinicians alike.
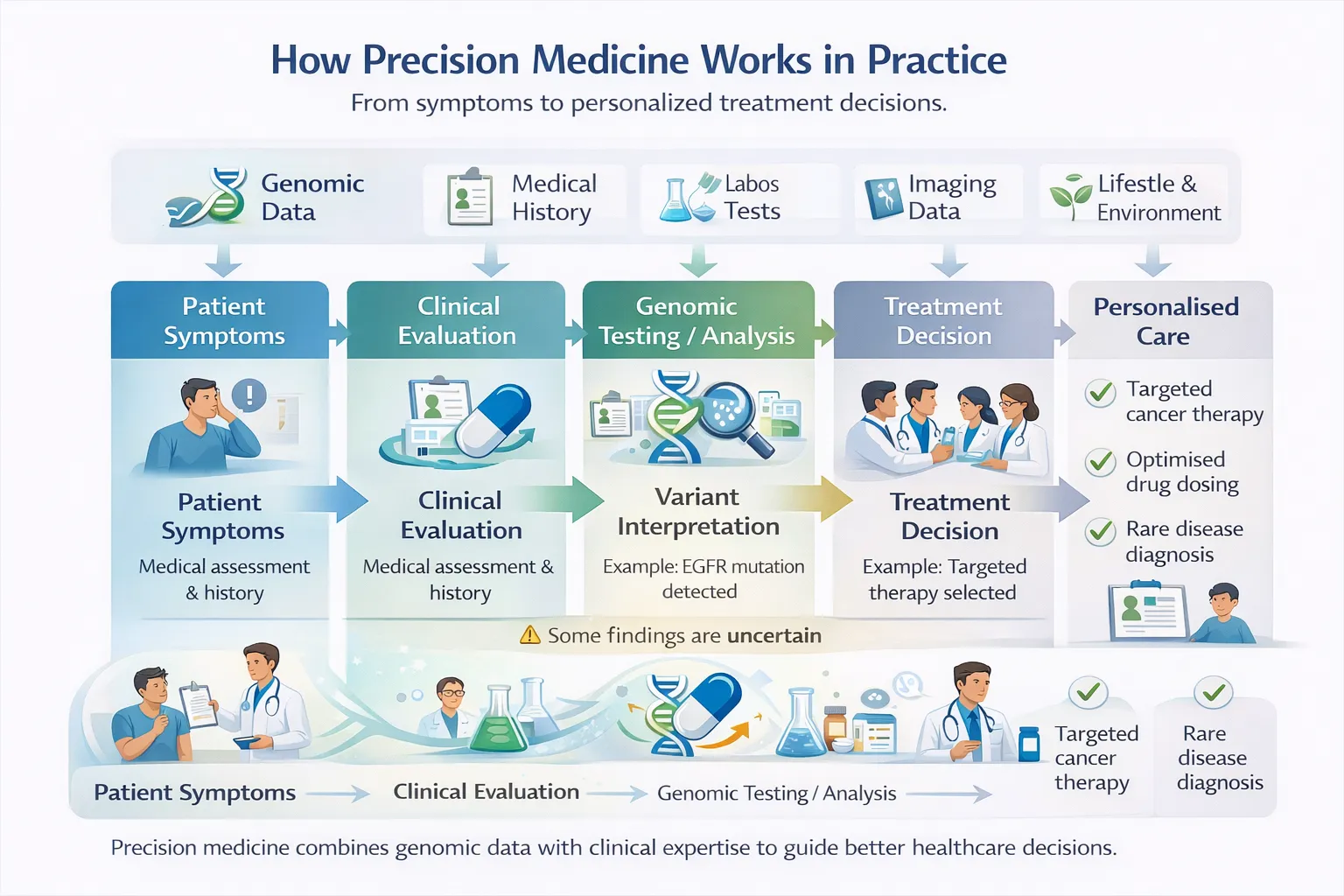
What Precision Medicine Can Do Today
1. Improve Drug Safety and Effectiveness
One of the clearest successes of precision medicine is pharmacogenomics—using genetic information to guide medication choice and dosing.
For some commonly used drugs, genetic differences affect:
- How quickly a drug is broken down
- Whether it works at all
- The risk of serious side effects
Clinical guidelines from groups such as the Clinical Pharmacogenetics Implementation Consortium help clinicians translate these results into prescribing decisions.
What this means for patients Fewer adverse reactions, less trial-and-error, and safer prescribing—especially for high-risk medications.
2. Guide Cancer Treatment More Precisely
In oncology, precision medicine has already changed standard care.
Tumours can now be classified not just by where they arise, but by:
- The mutations driving their growth
- Molecular pathways involved
- Likely resistance mechanisms
This allows some patients to receive targeted therapies matched to their tumour’s biology rather than broad chemotherapy.
Regulatory agencies such as the U.S. Food and Drug Administration have approved multiple therapies based on genomic tumour markers rather than cancer type alone.
What this means for patients For some cancers, treatment can be more effective and less toxic—and in certain cases, life-extending.
3. End Diagnostic Odysseys in Rare Disease
For individuals with rare or unexplained conditions, genomic sequencing has become a powerful diagnostic tool.
Whole-exome and whole-genome sequencing can:
- Identify previously unrecognized genetic disorders
- Provide long-sought explanations for symptoms
- Inform prognosis and family planning
Even when no cure exists, a diagnosis can still be profoundly meaningful.
What this means for patients Answers after years of uncertainty—and access to appropriate care, support, and information.
4. Improve Risk Stratification (in Some Contexts)
In certain conditions, combining genetic data with clinical factors can help identify people at higher or lower risk.
Examples include:
- Cardiovascular disease
- Some cancers
- Certain autoimmune conditions
This supports earlier monitoring or preventive strategies for selected individuals.
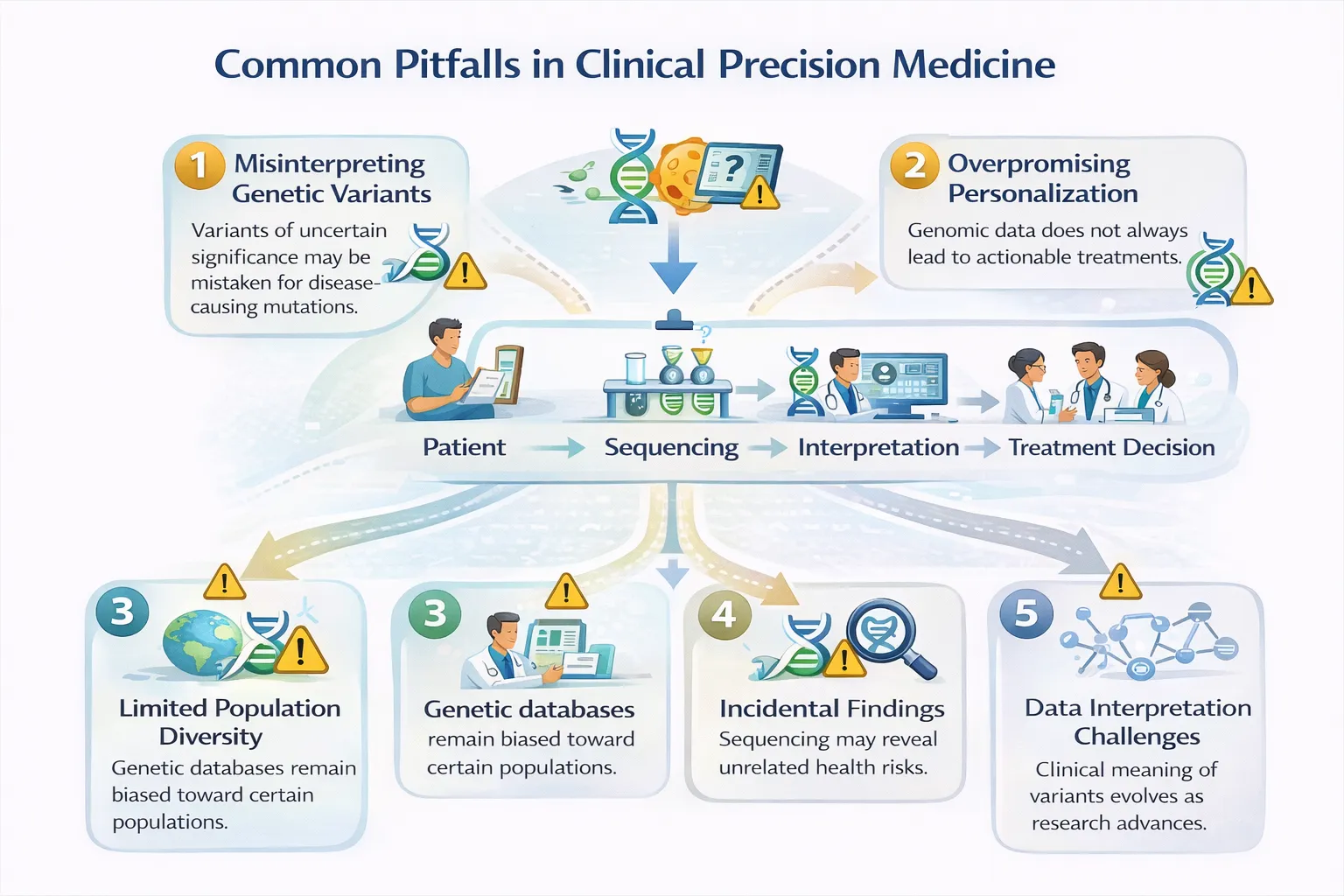
What Precision Medicine Cannot Do Yet
1. Predict Disease with Certainty
Genetic risk is probabilistic, not deterministic.
Most common diseases result from:
- Many genes acting together
- Environmental exposures
- Lifestyle and social factors
- Random biological variation
Even a “high genetic risk” does not mean disease is inevitable—and a low-risk result does not guarantee protection.
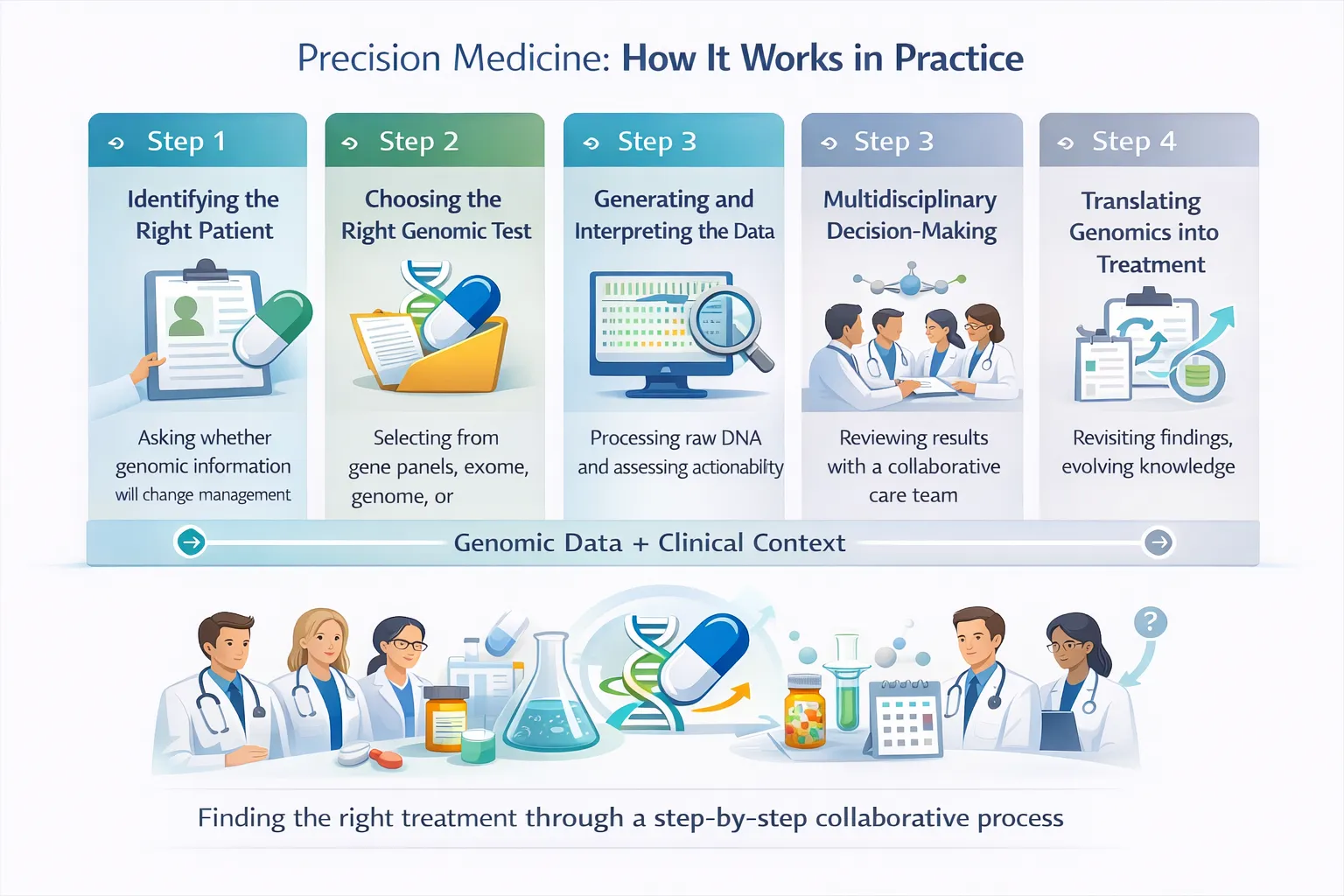
2. Personalize Care for Everyone (Yet)
Precision medicine works best when:
- There is strong scientific evidence
- The condition has a clear biological mechanism
- Actionable interventions exist
For many diseases, especially common chronic conditions, genomic information adds only limited clinical value—for now.
3. Eliminate Uncertainty
A significant proportion of genetic findings are classified as variants of uncertain significance (VUS).
This means:
- Science does not yet know whether the variant matters
- No treatment decisions should be based on it
- Reclassification may take years or never occur
Uncertainty is not a failure—it reflects the frontier of knowledge.
4. Replace Clinical Judgment
Precision medicine is sometimes described as “data-driven care.” In reality, it is decision-supported care.
Genomic information must always be interpreted alongside:
- Symptoms
- Physical findings
- Imaging and laboratory results
- Patient preferences and values
No genetic result should override clinical context.
5. Overcome Health Inequities Automatically
Genomic research has historically focused on populations of European ancestry.
As a result:
- Some tests perform better in certain groups than others
- Risk predictions may be less accurate for under-represented populations
- Uncertainty may be higher in diverse patients
Initiatives like the Human Pangenome Reference Consortium aim to address this, but equity remains an active challenge.
Why These Limits Matter
Understanding what precision medicine cannot do is just as important as celebrating what it can.
Over-promising leads to:
- Unrealistic expectations
- Disappointment or mistrust
- Inappropriate testing or treatment
Responsible precision medicine is:
- Evidence-based
- Transparent about uncertainty
- Integrated into whole-person care
The Bottom Line
Precision medicine is not magic—and it is not finished.
It is a powerful, evolving approach that:
- Improves care in specific, well-defined situations
- Adds meaningful insight without eliminating uncertainty
- Works best when paired with thoughtful clinical judgment
For patients, the promise of precision medicine is not perfection—it is better-informed care.
For clinicians, it is not replacement—it is reinforcement.
And for healthcare as a whole, it is a long-term shift toward understanding disease at a deeper, more human level.