Introduction
Imagine a world where your doctor prescribes a treatment specifically suited to your DNA, lifestyle, and environment. That’s precision medicine — a healthcare revolution enabled by post-genomic insights. Instead of applying the same therapy to everyone with a particular disease, precision medicine considers individual genetic differences, molecular profiles, and environmental factors to optimize outcomes.
This article explores how precision medicine works, its real-world applications, and the remarkable benefits it is already delivering to patients worldwide.
What is Precision Medicine?
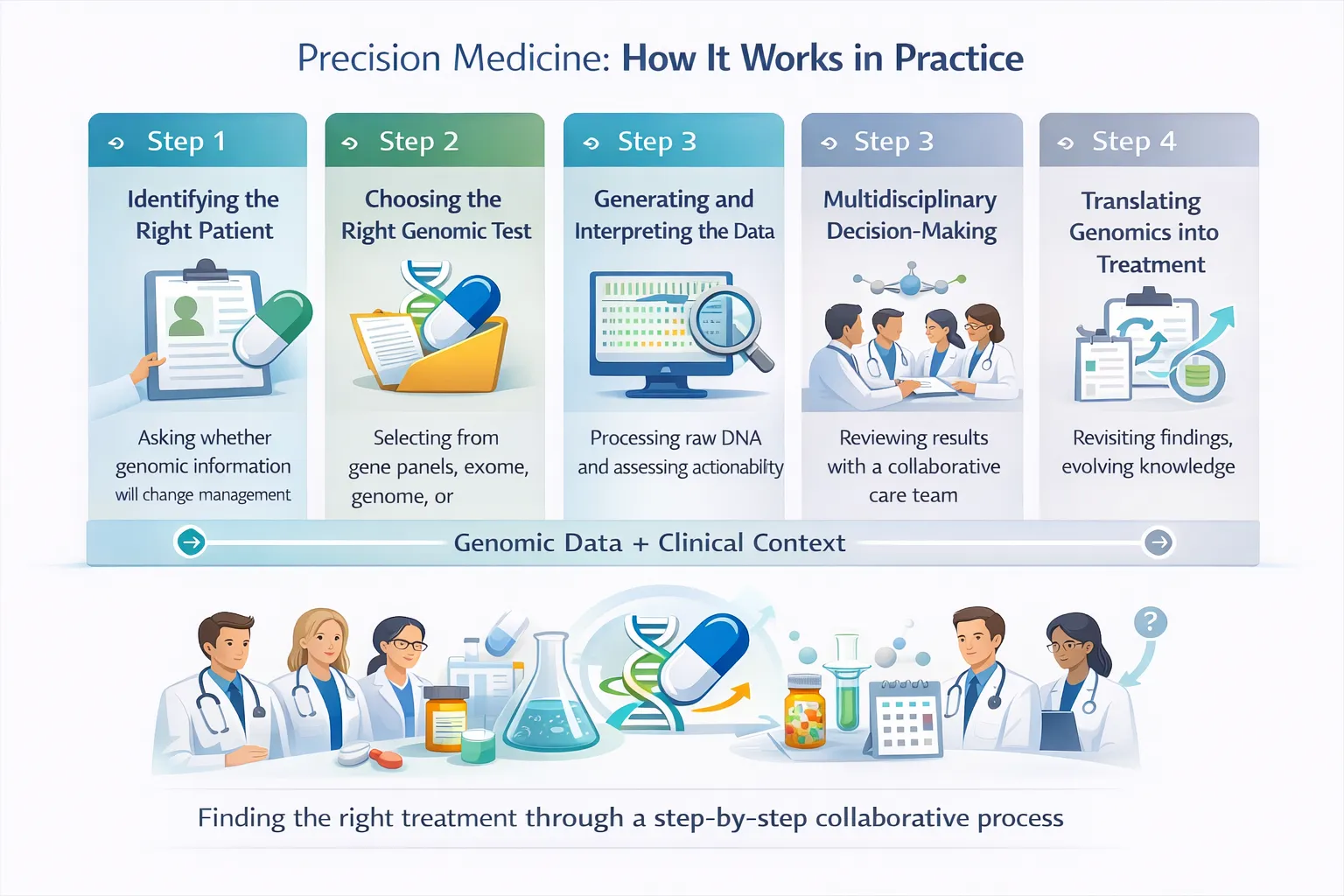
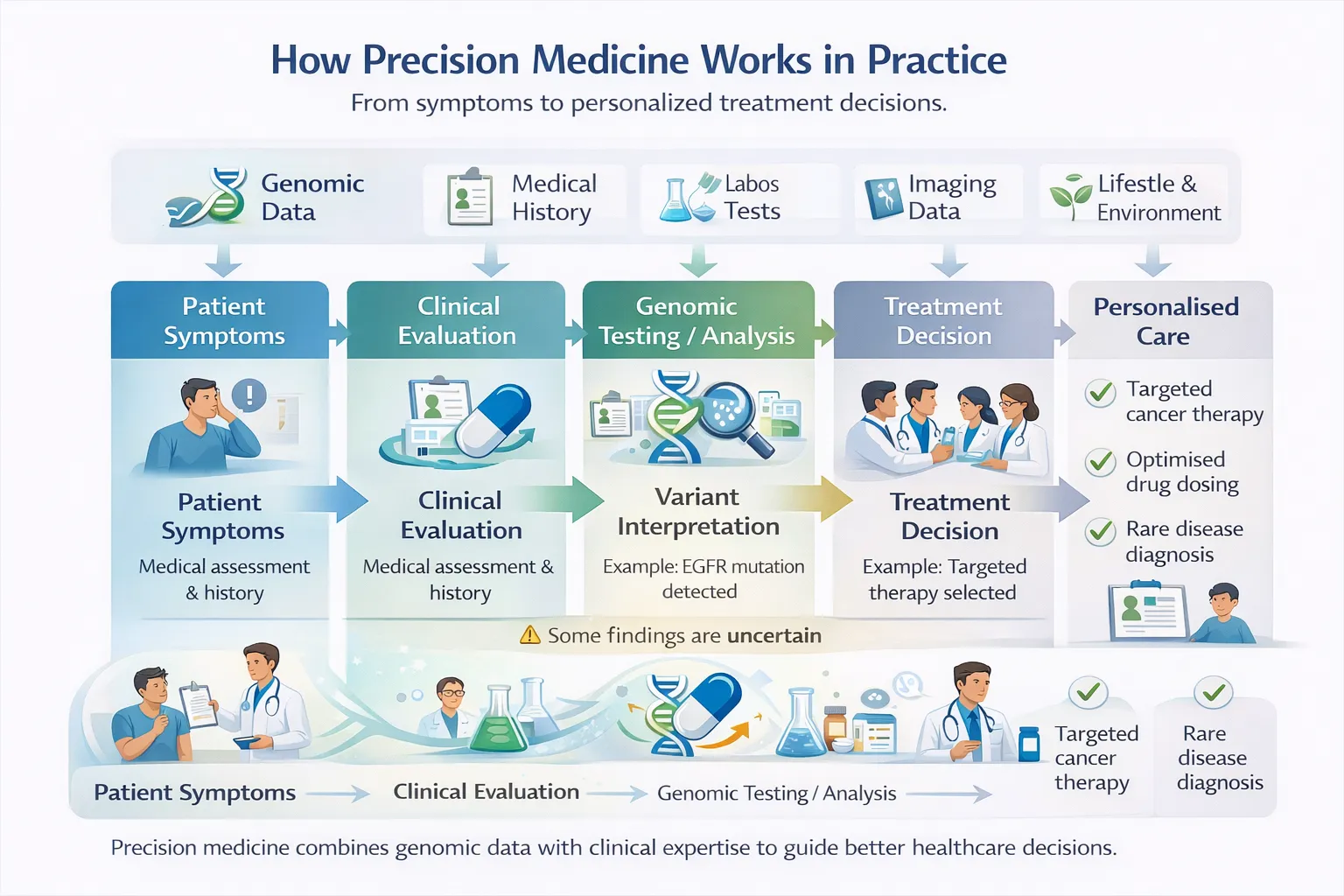
Precision medicine (sometimes called personalized medicine) is an approach where diagnosis, prevention, and treatment are customized to an individual patient. It relies on:
- Genomic data – DNA, RNA, epigenetics
- Clinical data – symptoms, lab results, imaging
- Environmental & lifestyle factors – diet, exposure, habits
📌 Key concept: Your DNA is not your destiny, but it can guide smarter, safer, and more effective healthcare decisions.
Real-World Clinical Examples
1. Pharmacogenomics: The Right Drug, the Right Dose
Pharmacogenomics studies how genetic variants affect drug metabolism. By understanding these variants, doctors can prescribe the right drug at the right dose for each patient.
Example:
- Clopidogrel (Plavix): Some patients have variants in the CYP2C19 gene that reduce the drug’s effectiveness. Knowing this in advance prevents heart attacks or strokes due to ineffective treatment (NEJM, 2009) .
- Warfarin: Genetic testing for CYP2C9 and VKORC1 variants helps tailor doses, reducing bleeding risks.
Public takeaway: Genetic testing can prevent serious side effects and improve treatment effectiveness. Clinician takeaway: Pharmacogenomics is now integrated into clinical decision support tools in hospitals and electronic health records.
2. Cancer Therapy: Targeted and Immunotherapy
Cancer is a genetic disease at its core. Precision medicine allows treatments to target specific mutations or molecular features of tumors rather than the tissue of origin alone.
Examples:
- EGFR mutations in lung cancer: Patients with these mutations respond dramatically to EGFR inhibitors (NEJM, 2004) .
- BRCA1/2 mutations in breast and ovarian cancer: Guide PARP inhibitor therapy (Lancet Oncol, 2017) .
- CAR-T therapy for leukemia: Patient T cells are engineered to target cancer cells, guided by molecular profiling (NEJM, 2014) .
Public takeaway: Tumors that look similar under a microscope can respond very differently depending on their genetic makeup. Clinician takeaway: Genomic profiling is now standard in many cancers to select targeted or immunotherapies.
3. Rare Disease Diagnostics: Ending the Diagnostic Odyssey
Millions of patients with rare conditions spend years without a definitive diagnosis. Precision medicine changes that.
Example:
- Whole-exome sequencing uncovers pathogenic variants causing rare metabolic or developmental disorders.
- Diagnostic yields of 30–50% in previously unsolved cases (JAMA, 2019) .
- Allows early intervention or tailored therapy, sometimes changing the disease course.
Public takeaway: Families finally get answers after years of uncertainty. Clinician takeaway: NGS pipelines are becoming standard in tertiary care for undiagnosed patients.
How Precision Medicine Benefits Patients
| Benefit | Example |
|---|---|
| Safer prescriptions | Pharmacogenomic-guided warfarin dosing |
| More effective therapies | Targeted cancer therapies based on tumor mutation |
| Faster diagnosis | Rare disease sequencing shortening the diagnostic odyssey |
| Preventive strategies | Polygenic risk scores identify high-risk patients for early intervention |
Challenges and Considerations
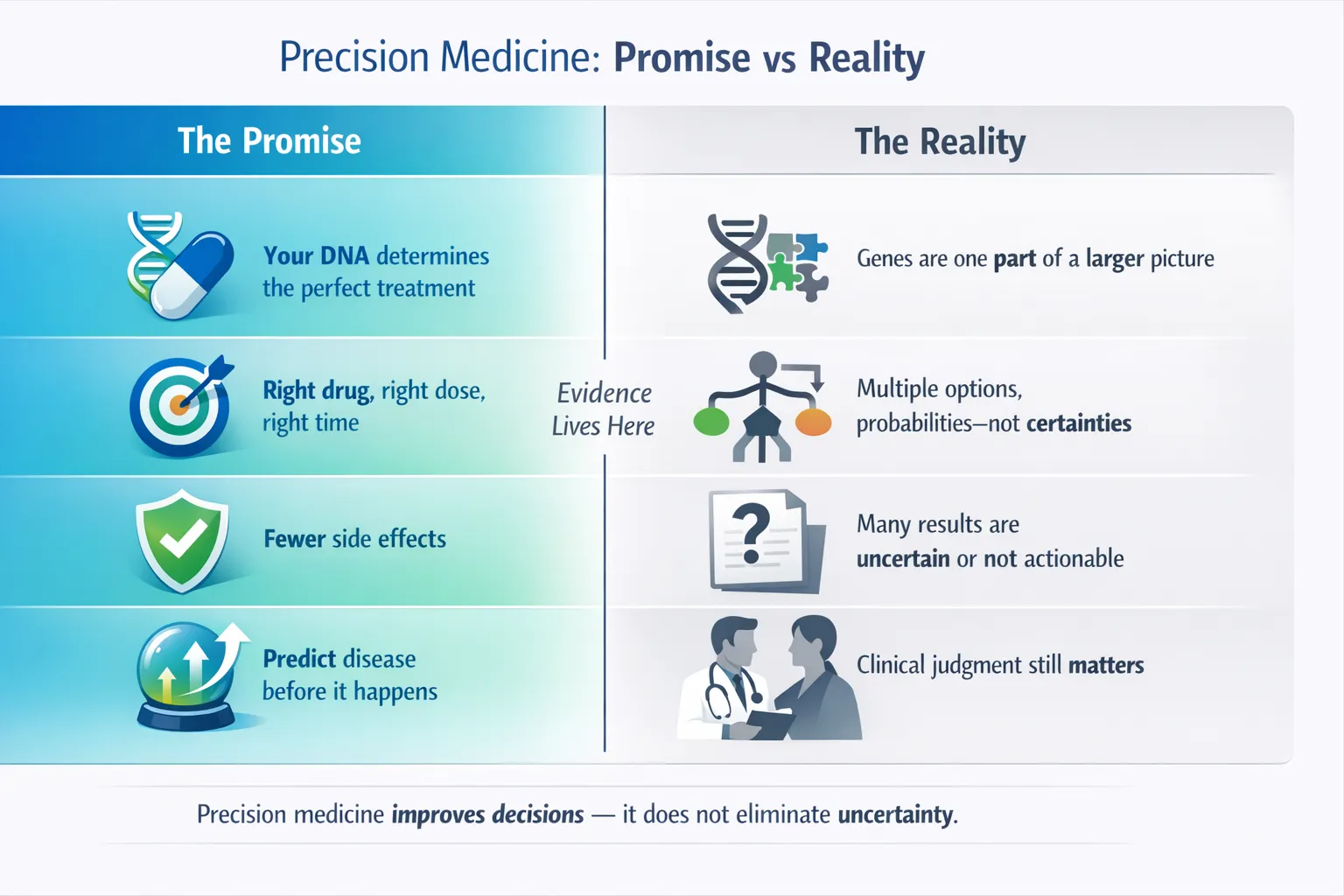
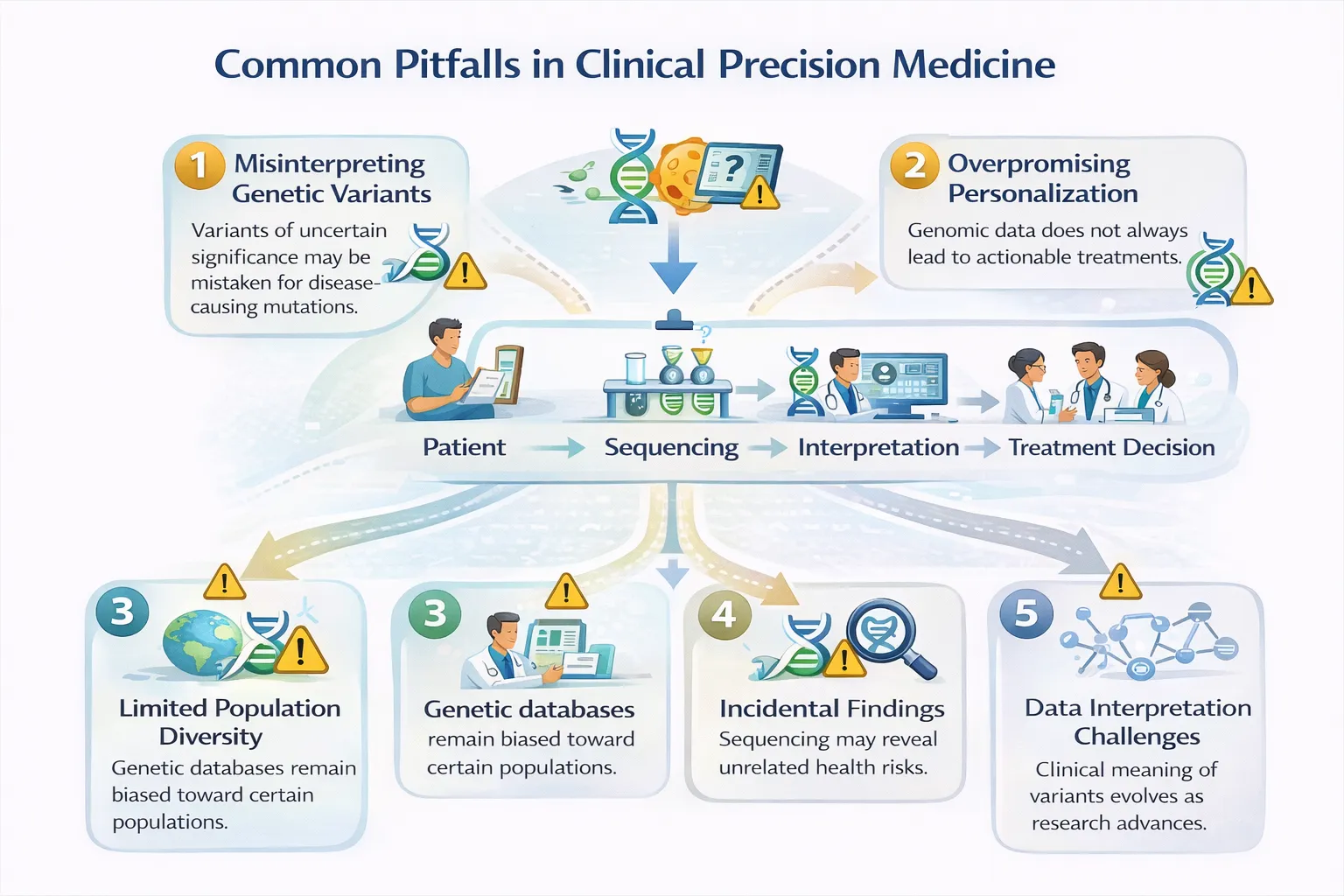
While precision medicine offers huge promise, clinicians must be aware of:
- Variants of uncertain significance (VUS) – not all genetic findings are actionable
- Population diversity gaps – reference genomes are still skewed toward European ancestries
- Cost and access – sequencing and testing remain expensive in some regions
- Ethical considerations – informed consent, data privacy, and insurance discrimination
Future Directions
- Integration with AI: Predict disease risk and treatment response using multi-omic datasets
- Preventive genomics: Using polygenic risk scores for early interventions in common diseases
- Global equity: Expanding precision medicine to underrepresented populations
Conclusion
Precision medicine is more than a scientific concept—it’s a clinical reality. From safer drug dosing to targeted cancer therapies and rare disease diagnostics, your DNA increasingly informs your healthcare journey. Both patients and clinicians benefit from smarter, tailored, and effective interventions that were unimaginable just 20 years ago.
Discover how polygenic risk scores predict disease risk in our next blog post: Polygenic Risk Scores: Can Your DNA Predict Your Health?